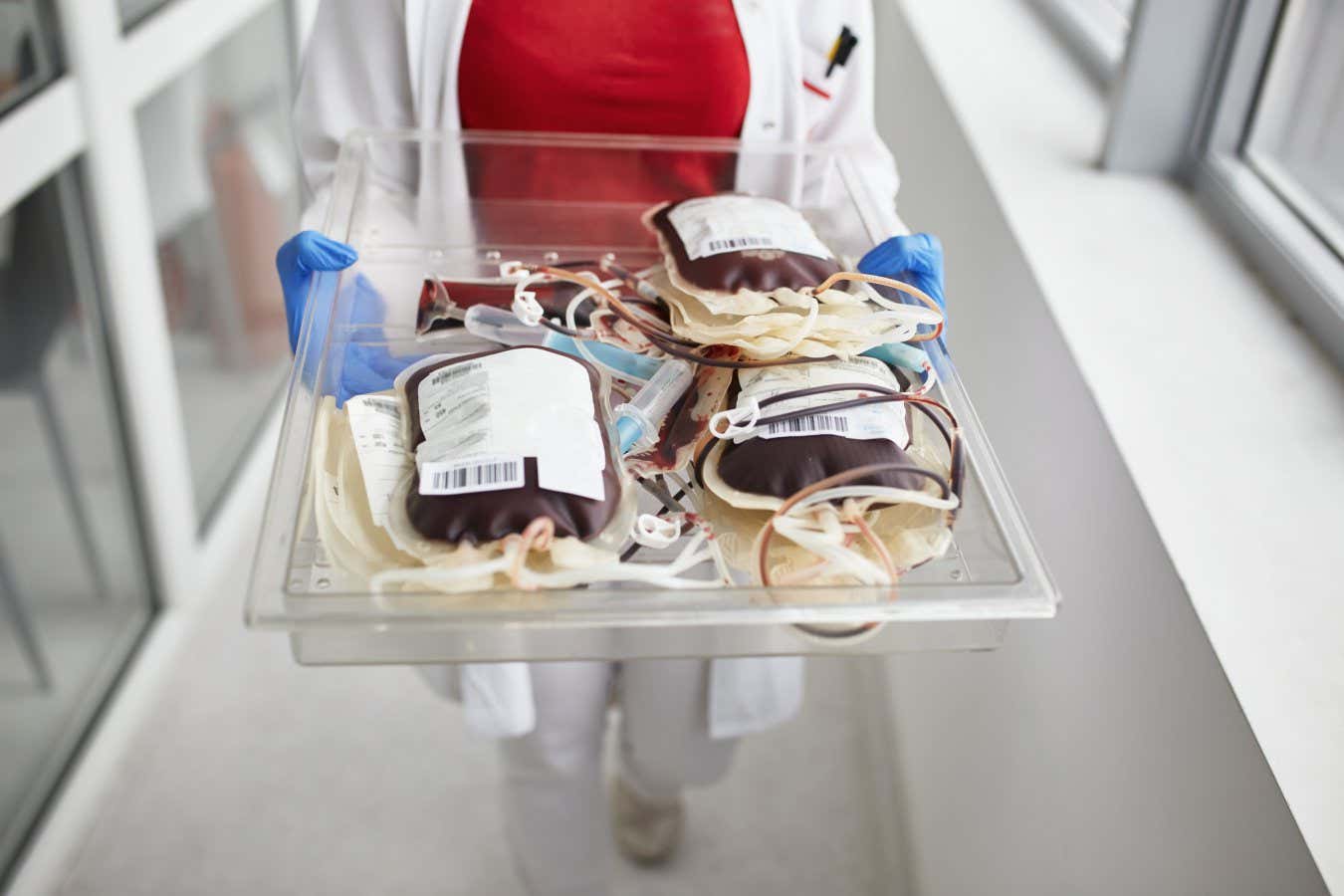
Donated blood usually comes from anonymous volunteers, and is screened for safety
Getty Images
A hospital in the US has had to concede to an unusual request from patients requiring blood transfusions: that they come from donors who haven’t been vaccinated against covid-19. This has led to delays in treatments that caused one individual to experience a life-threatening reaction.
“These requests were often driven by misinformation about vaccine safety and the blood supply, rather than evidence-based transfusion concerns,” says Jeremy Jacobs at Vanderbilt University Medical Center in Nashville, Tennessee. “I think one of the most important broader points is that the community blood supply is already highly regulated and carefully screened, and there is no evidence that requesting unvaccinated blood improves transfusion safety.”
Jacobs and his colleagues analysed blood donations that took place at the Vanderbilt centre between January 2024 and December 2025. They found that 15 patients – or their caregivers – had asked for directed donations, when blood is donated by a chosen person, often a relative, rather than being taken from a blood bank.
Directed donations are only permitted in the UK and Australia under exceptional circumstances, such as if an individual has a rare blood type and a suitable blood-bank donor isn’t available. In the US, the practice is allowed more broadly, but discouraged, with policies varying hugely between centres.
The researchers found that all 15 of the patients had directed donations because they wanted blood from a donor who they knew had not been vaccinated. This was specifically against covid-19, says Jacobs. The vaccination status of anonymised donors is not recorded or conveyed by blood banks.
These requests resulted in treatment delays that put the patients at risk. In the most extreme case, the patient’s level of haemoglobin – the protein that carries oxygen around the body – reached a critical level, which can cause organ injury and failure. Another patient developed anaemia.
“Directed donation is operationally more complex than using the routine blood supply,” says Jacobs. “It requires additional coordination, collection, processing, tracking and timing.”
Although blood is carefully screened before transfusion, direct donations have also been linked to a higher infection risk. This is because they are often given as a one-off, rather than coming from repeat donors in the community who may be known to blood banks and might be particularly cautious of their infection exposure.
Direct donations spiked during the HIV/AIDS epidemic during the 1980s and early 1990s, but they increased in prominence again when the mRNA covid-19 vaccines became available. These involve injecting part of SARS-CoV-2’s genetic code into someone so their cells produce one of its proteins. Their immune system then reacts and destroys cells with this protein. If the individual later catches SARS-CoV-2, their immune system is triggered to fight it off.
Research has repeatedly shown that these vaccines are safe and highly effective, but misinformation has incorrectly linked them to fertility problems and other health issues. Conspiracy theories have even wrongly stated that these vaccines contain a microchip and affect your DNA.
In 2025, a study confirmed that receiving blood donations from people vaccinated against covid-19 is safe. “Requests for unvaccinated blood reflect broader uncertainty about vaccines among a proportion of the public, rather than any recognised transfusion risk,” says Ash Toye at the University of Bristol, UK.
And the issue isn’t just affecting the Vanderbilt centre. The Welsh Blood Service stated last year that people are asking about the vaccination status of blood donors. There was also a rejected petition to the UK government to split blood donations by vaccination status. But in Oklahoma, legislators have proposed mandating that patients have access to unvaccinated blood.
“These requests illustrate how misinformation can create real operational burdens for patients, hospitals and blood providers,” says Jacobs. “At the same time, they underscore the importance of addressing patients’ concerns respectfully and thoughtfully, even when those concerns are not supported by evidence.”
Topics: